The head of the Department of Hemoblastosis and Hematopoietic Depression Chemotherapy of the NMRC for Hematology of the Ministry of Health of Russia, hematologist, Candidate of Medical Sciences, Zalina Fidarova talks about aplastic anemia using a clinical case as an example.
"Aplastic anemia is comparable in severity to tumor diseases of the blood system. With aplastic anemia the patient does not have his own erythrocytes, leukocytes, platelets, or the patient has very few of them. Minimal foci of hematopoiesis of the bone marrow are preserved, but this is not enough to ensure the vital activity of the body,”- says Zalina T. Fidarova
Clinical case-debut. Patient M., 23 years old. He was admitted to his local hospital with complaints of fever up to 40 degrees, general weakness, pain and inflammation in the rectum and gastrointestinal tract. The patient underwent massive antibacterial therapy and multiple transfusions of erythrocytes and platelets. Despite this, the condition did not improve. After a telemedicine consultation, the patient was transferred to the NMRC for Hematology.
The severity of the condition upon admission was due to deep agranulocytosis (leukocytes less than 200 cells), fever up to 40 degrees with chills, infectious complications: paraproctitis and mucositis of III-IV degree.
Acinetobacter baumannii resistant to antibacterial therapy was found in blood cultures. Under these conditions, immunosuppressive therapy, usually prescribed in the first line, was impossible due to the high risk of uncontrolled infectious complications and death. Promptly performed HLA-typing of the patient’s sister showed their incompatibility. Fortunately, the patient was stabilized and the course of antithymocytic globulin (ATG) was started.
 Z. T. Fidarova: "In most cases, patients are hospitalized in critically serious condition. The disease can begin with infectious complications, bleeding or pronounced weakness. After the necessary examination and confirmation of the diagnosis, immunosuppressive therapy or bone marrow transplantation from a related fully compatible donor in the first line of therapy is indicated. Unlike tumor diseases where chemotherapy is used, immunosuppressive therapy is used for the treatment of aplastic anemia. Therefore, it is very important that patients do not have severe infections at the time of treatment. Due to the absence of leukocytes, severe infectious complications often occur at the onset of the disease. Any microorganisms that normally live in the oral cavity or in the intestine and do not pose a danger to a healthy person, become aggressive with aplastic anemia. Patients often develop a high fever, with a risk of developing sepsis."
Z. T. Fidarova: "In most cases, patients are hospitalized in critically serious condition. The disease can begin with infectious complications, bleeding or pronounced weakness. After the necessary examination and confirmation of the diagnosis, immunosuppressive therapy or bone marrow transplantation from a related fully compatible donor in the first line of therapy is indicated. Unlike tumor diseases where chemotherapy is used, immunosuppressive therapy is used for the treatment of aplastic anemia. Therefore, it is very important that patients do not have severe infections at the time of treatment. Due to the absence of leukocytes, severe infectious complications often occur at the onset of the disease. Any microorganisms that normally live in the oral cavity or in the intestine and do not pose a danger to a healthy person, become aggressive with aplastic anemia. Patients often develop a high fever, with a risk of developing sepsis."
Clinical case - treatment. Against the background of the introduction of ATG, the condition deteriorated sharply. The development of sepsis associated with Acinetobacter baumannii was noted. The patient was brought out of the septic state by combining several antibacterial drugs, however, the spread of microorganisms led to the development of multiple foci of abscesses of the soft tissues of the thigh and buttock area. Joints were also affected, which was accompanied by a pronounced pain syndrome. Treatment was further complicated by low blood counts (leukocytes less than 500 cells).
The hematopoiesis stimulator eltrombopag was added to the therapy. After that, the patient responded to treatment, leukocytes recovered, a granulocyte sprout appeared in the bone marrow, thanks to which infectious complications were controlled.
After some time, the infiltrates were drained and areas of dead muscle tissue were surgically removed. The recovery was carried out with the help of a VAC system. The postoperative wounds were carefully treated with the bandages changed daily.
Z. T. Fidarova: "Sepsis is a severe infectious complication in which bacteria spread with the blood flow through the internal organs. In the case of our patient, the targets were muscles and joints. Fortunately, thanks to the treatment, the bone marrow has restored its function and the patient has his own white blood cells. The infiltrates in the muscles have thickened enough so that they can be opened, drained and suppuration removed. The wounds have completely healed. Before, the course of antithymocytic globulin was not given to patients with infectious complications, now thanks to the advent of new antibacterial drugs and an experienced team of resuscitators and surgeons, we can do it."
Clinical case- results. The treatment took five months. During all this time, the patient underwent transfusions of donor platelets and erythrocytes, which made it possible to conduct adequate treatment. In addition to hematologists, specialists like bacteriologists, surgeons, and anesthesiologists also took a part in the treatment. A minimal response was achieved. There is hope for stabilization of the condition in the near future and the onset of partial or complete remission. Despite massive surgical intervention, all muscle motor functions were preserved.
The patient was discharged in a satisfactory condition. Currently, the dependence on transfusions of donor platelets remains. The patient continues to receive minimal doses of immunosuppressive therapy. Doctors hope that over time it will be possible to abandon transfusions of blood components and completely cancel immunosuppressive therapy.
Z. T. Fidarova: "We are actively studying aplastic anemia and continue to search for effective treatment methods. We hope to be able to help more patients with this serious disease soon."
Reference. Acquired aplastic anemia is a disease of the blood system characterized by a decrease in the hematopoietic function of the bone marrow and is manifested by insufficient formation of shaped blood elements: erythrocytes, leukocytes and platelets. According to the Federal Register of Life-Threatening and Chronic Progressive Rare (Orphan) Diseases, 1,259 patients with aplastic anemia were registered in 2020. Aplastic anemia has two peaks of incidence: 20-25 years and 60-65 years.
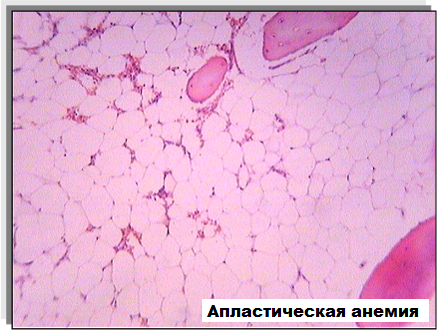 The treatment program for the acquired form of aplastic anemia includes combined immunosuppressive therapy using antithymocytic globulin (ATG) and cyclosporine and (for young patients) transplantation of hematopoietic stem cells (bone marrow) from a related fully compatible donor. However, the percentage of transplantation does not exceed 10% due to the absence of a related compatible donor in most patients. In rare cases, an unrelated compatible donor is considered. For patients of the older age group, bone marrow transplantation is not performed, since the risk of its implementation is associated with severe complications, and the result is comparable to immunosuppressive therapy. Thus, in most cases, combined immunosuppressive therapy remains the therapy of choice.
The treatment program for the acquired form of aplastic anemia includes combined immunosuppressive therapy using antithymocytic globulin (ATG) and cyclosporine and (for young patients) transplantation of hematopoietic stem cells (bone marrow) from a related fully compatible donor. However, the percentage of transplantation does not exceed 10% due to the absence of a related compatible donor in most patients. In rare cases, an unrelated compatible donor is considered. For patients of the older age group, bone marrow transplantation is not performed, since the risk of its implementation is associated with severe complications, and the result is comparable to immunosuppressive therapy. Thus, in most cases, combined immunosuppressive therapy remains the therapy of choice.
The effectiveness of treatment consists in achieving independence from transfusions of donor erythrocytes and platelets and restoring the number of neutrophils. When the patient's bone marrow begins to function, the patient’s own red blood cells, white blood cells and platelets appear in the blood.
In 50% of patients, immunosuppressive therapy leads to independence from transfusions after three months of treatment. In the another 25%, this happens after a repeated course of ATG. During all this time, patients need components of donated blood. In some patients, immunosuppressive therapy is ineffective. In this case the thrombopoietin receptor activator eltrombopag is included in the treatment program.
Aplastic anemia has no specific symptoms. All of them are somehow associated with bone marrow insufficiency and low blood cell counts. The disease can begin with increasing weakness, causeless bruises, gingival bleeding and persistent infections. A clinical blood test demonstrates three-stage cytopenia, that is, a decrease in all indicators of blood cells, after which targeted diagnostics begins.
 Diagnostics: morphological and standard cytogenetic examination of bone marrow cells, fish-examination of bone marrow cells, peripheral blood immunophenotyping.
Diagnostics: morphological and standard cytogenetic examination of bone marrow cells, fish-examination of bone marrow cells, peripheral blood immunophenotyping.
Aplastic anemia is a diagnosis of exclusion. This means that the choice is made between several diseases with similar symptoms by the method of exclusion on certain grounds. In the case of aplastic anemia, differential diagnosis is carried out between tumor diseases of the blood system, myelodysplastic syndrome, vitamin B12 deficiency, systemic collagenosis, tuberculosis and hepatitis-associated bone marrow aplasia. The treatment of congenital and acquired forms of aplastic anemia is radically different.
The causes of acquired aplastic anemia are not exactly known. The influence of factors such as medication, contact with organic solvents, arsenic compounds and pesticides has not been proven. The immediate cause most often remains unknown.
The prognosis in patients with aplastic anemia is favorable. The overall survival rate for 10 years is 85-90%. Long-term monitoring is required, including a standard cytogenetic study of the bone marrow.


